Perioperative cardiac risk management focuses on minimizing cardiovascular complications in patients undergoing noncardiac surgery, a multifaceted and crucial discipline․
Scope of the Guidelines
These guidelines comprehensively address the perioperative evaluation and management of cardiac risk in patients undergoing noncardiac surgical procedures․ They aim to standardize care, improving outcomes and reducing adverse cardiovascular events․ The focus extends to all adult patients, acknowledging the increasing prevalence of underlying cardiac conditions․
The guidelines cover preoperative assessment, risk stratification utilizing tools like RCRI and NSRSC, and optimization of pre-existing conditions․ Intraoperative monitoring, anesthetic considerations, and postoperative cardiac care are also detailed․ Furthermore, the integration of Enhanced Recovery After Surgery (ERAS) cardiac protocols is emphasized, promoting multimodal analgesia and early mobilization for improved patient recovery․
Importance of Risk Stratification
Accurate risk stratification is paramount in perioperative cardiac care, as patients undergoing noncardiac surgery face significant cardiovascular risks․ Identifying those at higher risk allows for tailored interventions, optimizing their condition before, during, and after the procedure․ Unrecognized myocardial infarctions are surprisingly common, with potentially up to half going undetected․
Tools like the Revised Cardiac Risk Index (RCRI) and National Surgical Risk Calculator (NSRSC) aid in this process, alongside ACC/AHA guidelines․ A stepwise approach, guided by these assessments, helps clinicians determine if surgery should proceed and informs the intensity of cardiac monitoring and medical optimization needed to mitigate potential complications․
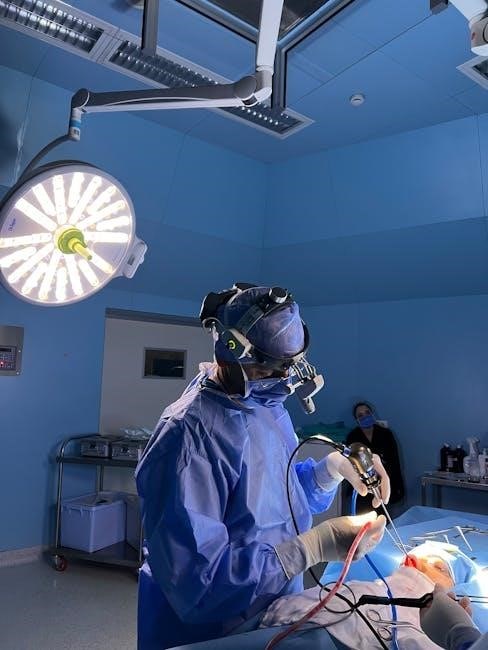
Preoperative Evaluation
A careful clinical risk evaluation, including patient history, physical exam, ECG, and biomarkers, is essential before noncardiac surgery to assess cardiac status․
Patient History and Physical Examination
A thorough patient history is the cornerstone of preoperative cardiac assessment․ Clinicians should meticulously document pre-existing cardiovascular conditions, including coronary artery disease, heart failure, and arrhythmias; Detailed questioning regarding symptom severity, functional capacity, and prior cardiac events is crucial․ The physical examination should focus on identifying signs of heart failure, such as edema and jugular venous distension, as well as assessing peripheral pulses and auscultating for murmurs․ Recognizing these factors helps stratify risk and guide further evaluation․ A stepwise approach to perioperative management relies heavily on this initial assessment, ensuring appropriate preparation for surgery and minimizing potential complications․
Electrocardiogram (ECG) Interpretation
Electrocardiogram (ECG) interpretation is vital in perioperative cardiac evaluation, aiding in the detection of ischemia, arrhythmias, and left ventricular hypertrophy․ Baseline ECGs should be obtained for all patients undergoing noncardiac surgery, particularly those with known cardiovascular disease or risk factors․ Identifying prior myocardial infarctions, bundle branch blocks, or significant ST-segment abnormalities is crucial․ Serial ECGs may be necessary for patients with concerning findings or those undergoing high-risk procedures․ Accurate interpretation, combined with clinical context, informs risk stratification and guides appropriate management strategies, ultimately improving patient safety during the perioperative period․
Biomarker Assessment (Troponin, BNP)
Biomarker assessment, specifically troponin and B-type natriuretic peptide (BNP), plays an increasingly important role in perioperative cardiac risk stratification․ Elevated troponin levels can indicate myocardial injury, even in the absence of classic ischemic symptoms, with up to 50% of perioperative MIs potentially unrecognized․ BNP levels correlate with ventricular stress and can help identify patients at risk for heart failure complications․ While not routinely recommended for all patients, biomarker assessment is valuable in those with intermediate or high-risk profiles, guiding further evaluation and management decisions to optimize outcomes․

Risk Stratification Tools
Utilizing tools like RCRI, NSRSC, and ACC/AHA guidelines enables a stepwise approach to assess surgical risk and optimize patient care effectively․
Revised Cardiac Risk Index (RCRI)
The Revised Cardiac Risk Index (RCRI) is a widely used, simple tool for pre-operative cardiac risk stratification in patients undergoing non-cardiac surgery․ It incorporates six independent predictors of major cardiac events: history of ischemic heart disease, prior heart failure, cerebrovascular disease, chronic kidney disease, diabetes mellitus requiring insulin treatment, and a pre-operative hemoglobin level less than 14 g/dL in men or 13 g/dL in women․
Each risk factor present contributes one point, resulting in a total score ranging from 0 to 6․ Higher RCRI scores correlate with an increased risk of post-operative cardiac complications, guiding clinical decision-making regarding further cardiac evaluation and optimization before surgery․
National Surgical Risk Calculator (NSRSC)
The National Surgical Risk Calculator (NSRSC), developed by the Veterans Affairs (VA) and American College of Surgeons (ACS), offers a more comprehensive assessment of perioperative risk․ Unlike the RCRI, the NSRSC utilizes a complex algorithm incorporating 19 variables, including age, sex, race, and various pre-existing conditions like heart failure, chronic lung disease, and renal insufficiency․
It predicts the risk of 30-day mortality and major cardiac events, providing a more individualized risk profile․ The NSRSC is particularly valuable for patients undergoing higher-risk procedures, aiding in shared decision-making and optimizing pre-operative preparation․
American College of Cardiology/American Heart Association (ACC/AHA) Guidelines
The American College of Cardiology (ACC) and American Heart Association (AHA) collaboratively released clinical practice guidelines for perioperative cardiovascular evaluation and management․ These guidelines emphasize a stepwise approach, advocating for a thorough assessment of cardiac risk based on the type of surgery and patient comorbidities․
They recommend utilizing risk indices like the RCRI and NSRSC, alongside clinical judgment, to determine the need for further cardiac testing․ The ACC/AHA guidelines prioritize optimizing pre-existing cardiac conditions and tailoring anesthetic plans to minimize cardiovascular stress during and after surgery․
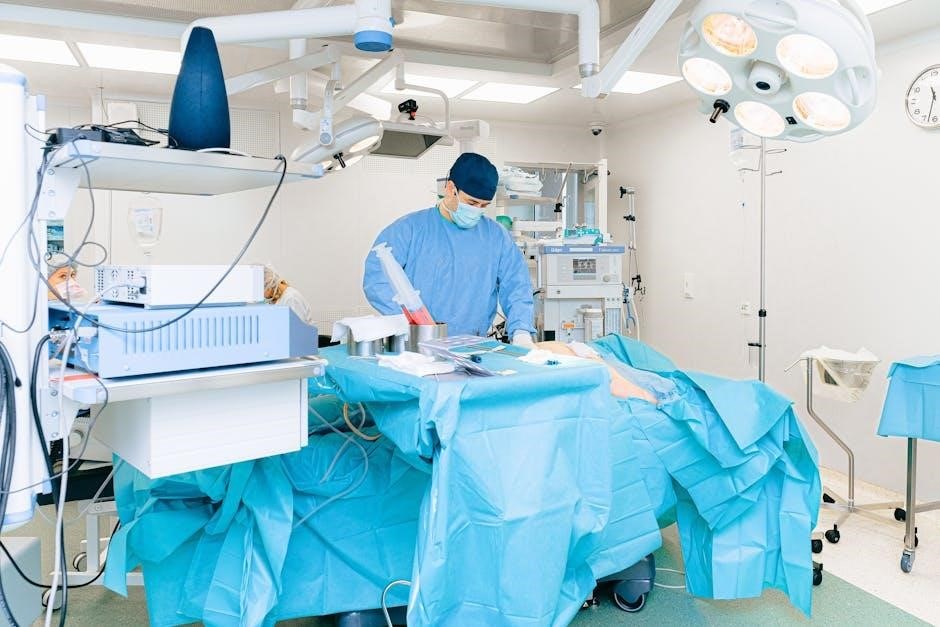
Management of Pre-existing Cardiac Conditions
Optimizing pre-existing conditions—coronary artery disease, heart failure, and arrhythmias—is paramount before noncardiac surgery to mitigate potential cardiovascular risks․
Coronary Artery Disease – Medical Optimization
Patients with established coronary artery disease require meticulous medical optimization prior to noncardiac surgery․ This involves continuing beta-blockers and statins, as abrupt discontinuation can elevate cardiac risk․ Angiotensin-converting enzyme inhibitors (ACEIs) or angiotensin receptor blockers (ARBs) should generally be continued, unless concerns about intraoperative hypotension exist․
Careful assessment of angina status is crucial; recent or ongoing angina warrants further evaluation, potentially including stress testing․ If possible, elective surgery should be postponed until angina is stable․ Consideration should be given to optimizing antiplatelet therapy based on individual bleeding risk and the planned surgical procedure; Thorough risk stratification is essential to guide these decisions․
Heart Failure – Diuretic and Inotropic Management
Patients with heart failure necessitate careful volume status assessment and optimization before surgery․ Diuretic management should aim for euvolemia, avoiding both overload and dehydration․ Continue guideline-directed medical therapy, including ACE inhibitors/ARBs, beta-blockers, and mineralocorticoid receptor antagonists, unless clinically contraindicated․
Inotropic support, while potentially beneficial in severe heart failure, carries risks and should be reserved for carefully selected patients․ Preoperative optimization includes addressing electrolyte imbalances and renal function․ Close monitoring of hemodynamics during surgery is paramount, with a low threshold for intervention if signs of decompensation arise․
Arrhythmias – Rate and Rhythm Control
Preoperative assessment should identify patients at risk for arrhythmias, including those with a history of atrial fibrillation or other rhythm disturbances․ Continue beta-blockers in patients already prescribed them, as abrupt cessation can precipitate tachycardia or ischemia․ Rate control is generally preferred over rhythm control in the perioperative period, minimizing the risk of pro-arrhythmic effects․
Avoidance of electrolyte imbalances (potassium, magnesium) is crucial․ Intraoperative bradycardia should be addressed promptly with anticholinergic agents or temporary pacing if necessary․ Postoperative atrial fibrillation is common; consider a lenient approach to rate control unless hemodynamically significant․
Intraoperative Monitoring
Continuous ECG, arterial blood pressure, and potentially CVP monitoring are essential during surgery to detect and manage cardiovascular instability promptly․
Continuous ECG Monitoring
Continuous electrocardiogram (ECG) monitoring is paramount throughout the perioperative period, serving as the cornerstone for detecting arrhythmias, ischemic changes, and conduction abnormalities․ This vigilant surveillance allows for the early identification of potentially life-threatening cardiac events, enabling timely intervention․
The ECG should be meticulously reviewed for signs of myocardial ischemia, such as ST-segment elevation or depression, and T-wave inversions․ Prompt recognition of arrhythmias – including atrial fibrillation, ventricular tachycardia, and bradycardia – is crucial for initiating appropriate treatment strategies․
Furthermore, continuous ECG monitoring aids in assessing the effectiveness of interventions and guiding hemodynamic management during surgery, ultimately optimizing patient safety and outcomes․
Arterial Blood Pressure Monitoring
Real-time arterial blood pressure (ABP) monitoring is essential for guiding fluid management and assessing cardiovascular function during surgery․ It provides a precise and continuous measure of systemic blood pressure, surpassing the limitations of non-invasive techniques․
Maintaining adequate blood pressure is critical for ensuring sufficient organ perfusion, particularly during periods of hemodynamic instability or significant blood loss․ ABP monitoring facilitates the titration of vasoactive medications to optimize cardiac output and systemic vascular resistance․
Early detection of hypotension or hypertension allows for prompt corrective measures, minimizing the risk of end-organ damage and improving overall patient outcomes․
Central Venous Pressure (CVP) Monitoring
Central venous pressure (CVP) monitoring offers valuable insights into right atrial pressure and, consequently, fluid status and cardiac function during surgery․ While its role has evolved with advanced hemodynamic monitoring techniques, CVP remains a useful adjunct in specific clinical scenarios․
CVP measurements assist in assessing the patient’s response to fluid resuscitation and guide the administration of intravenous fluids to maintain adequate preload․ However, it’s crucial to interpret CVP values in conjunction with other hemodynamic parameters․
Isolated CVP readings can be misleading; therefore, a comprehensive assessment is vital for optimal patient management․
Anesthetic Considerations
Careful selection of anesthetic agents and meticulous hemodynamic management are paramount during surgery to optimize cardiac function and prevent complications․
Choice of Anesthetic Agents
Selecting appropriate anesthetic agents is critical for perioperative cardiac care, demanding a nuanced understanding of their hemodynamic effects․ Volatile anesthetics, while offering advantages in recovery, can induce myocardial depression and should be used cautiously in vulnerable patients․ Intravenous agents like propofol provide stable hemodynamics but may exacerbate hypotension․
Regional anesthesia, when feasible, minimizes systemic effects and is often preferred․ Opioids, while valuable for analgesia, can cause histamine release and potentially compromise cardiovascular stability․ A balanced anesthetic approach, tailored to the patient’s cardiac status and surgical demands, is essential․
Hemodynamic Management During Surgery
Maintaining optimal hemodynamics during surgery is paramount, requiring vigilant monitoring and proactive intervention․ Careful fluid management is crucial, avoiding both hypovolemia and excessive fluid overload, which can strain the cardiovascular system․ Vasopressors, such as phenylephrine or norepinephrine, may be necessary to support blood pressure, but should be titrated cautiously․
Inotropic support, like dobutamine, can enhance cardiac output in patients with compromised ventricular function․ Avoiding significant fluctuations in heart rate and blood pressure is key, as these can precipitate ischemia․ A collaborative approach between the surgeon and anesthesiologist is vital for effective hemodynamic control․
Prevention of Hypothermia
Maintaining normothermia throughout the surgical procedure is essential, as hypothermia significantly increases the risk of cardiac complications․ Active warming techniques, including forced-air warming blankets and warmed intravenous fluids, should be employed proactively․ Monitoring core body temperature continuously allows for timely intervention․
Insulation with appropriate coverings minimizes heat loss to the environment․ Careful consideration of the surgical site and exposure time is also important; Avoiding excessive irrigation with cold fluids further contributes to thermal stability․ Preventing hypothermia optimizes cardiovascular function and reduces the incidence of adverse events․
Postoperative Cardiac Care
Postoperative care prioritizes early detection of complications, managing arrhythmias, and preventing myocardial infarction for optimal patient recovery and reduced cardiovascular risk․
Early Detection of Cardiac Complications
Vigilant monitoring postoperatively is paramount for identifying cardiac issues promptly․ This includes continuous ECG surveillance to detect arrhythmias or ischemic changes, alongside frequent assessment of vital signs – blood pressure, heart rate, and oxygen saturation․
Clinicians should maintain a high index of suspicion for silent myocardial infarctions, as up to 50% may go unrecognized․ Serial biomarker assessments, specifically troponin levels, are crucial for detecting myocardial damage․
Prompt investigation of any new or worsening chest pain, dyspnea, or hemodynamic instability is essential․ Early identification allows for timely intervention, improving patient outcomes and minimizing long-term cardiovascular consequences․
Management of Postoperative Arrhythmias
Postoperative arrhythmias are common, often transient, but require careful evaluation and management․ Initial steps involve identifying and addressing underlying contributing factors, such as electrolyte imbalances, hypoxemia, or pain․
For stable arrhythmias, a conservative approach with frequent monitoring may suffice․ However, symptomatic or hemodynamically significant arrhythmias necessitate prompt intervention․
Pharmacological options include beta-blockers for supraventricular tachycardias and antiarrhythmic drugs for ventricular arrhythmias, guided by established protocols․ Cardioversion may be required for unstable rhythms․
Prevention of Postoperative Myocardial Infarction
Preventing postoperative myocardial infarction (MI) relies on comprehensive risk assessment and mitigation strategies․ Optimal medical management of pre-existing coronary artery disease is paramount, including continued beta-blocker therapy and statin use․
Maintaining hemodynamic stability during surgery, avoiding hypotension and hypoxemia, is crucial․ Judicious fluid management and avoidance of excessive surgical stress are also important preventative measures․
Early detection of cardiac ischemia through continuous ECG monitoring and biomarker assessment allows for timely intervention․ Postoperative monitoring for signs of MI remains essential for optimal patient outcomes․
Enhanced Recovery After Surgery (ERAS) Cardiac Protocols
ERAS Cardiac Society guidelines offer evidence-based protocols to enhance patient recovery post-surgery, focusing on multimodal analgesia, early mobilization, and optimized nutrition․
ERAS Cardiac Society Guidelines
The ERAS Cardiac Society has spearheaded the development of comprehensive guidelines, born from a rigorous two-year process, dedicated to elevating patient recovery within cardiac surgical programs․ These recommendations aren’t arbitrary; they are firmly rooted in evidence-based protocols, aiming to standardize and optimize care․ The core philosophy centers around a multimodal approach, acknowledging the interconnectedness of physiological systems․
Key components include meticulous preoperative optimization, minimized surgical stress, and proactive postoperative management․ This collaborative effort, involving leading heart surgeons, anesthesiologists, and critical care specialists, signifies a commitment to improving outcomes and enhancing the patient experience throughout the entire perioperative journey․
Multimodal Analgesia
A cornerstone of Enhanced Recovery After Surgery (ERAS) protocols is the implementation of multimodal analgesia, a strategy designed to minimize opioid consumption and improve pain control․ This approach moves beyond relying solely on strong opioids, integrating various analgesic techniques to target different pain pathways․
Techniques include preemptive analgesics, regional anesthesia, non-opioid medications like NSAIDs and gabapentinoids, and nerve blocks․ By combining these methods, clinicians can achieve superior pain relief with fewer side effects, facilitating earlier mobilization and improved patient satisfaction․ This holistic approach is vital for optimizing recovery post-cardiac surgery․
Early Mobilization and Nutrition
ERAS Cardiac Society guidelines strongly advocate for early mobilization and optimized nutrition as integral components of postoperative recovery following cardiac surgery․ Prompt ambulation, initiated as soon as clinically feasible, helps prevent complications like pneumonia, deep vein thrombosis, and muscle weakness․
Nutritional support, including early enteral feeding, is crucial to restore metabolic function and promote wound healing․ Protocols emphasize a proactive approach to addressing nutritional deficiencies and maintaining adequate caloric intake․ These interventions, combined with multimodal analgesia, contribute to faster recovery times and improved patient outcomes․

